Flashes and Floaters Introduction
This is one of the most common presentations in ophthalmology and is almost always due to the vitreous gel collapsing in on itself and peeling away from the retina, a process we call ‘posterior vitreous detachment’ or PVD for short.
This is a normal ageing process but can cause problems in some patients. About half of patients have no symptoms whatsoever when this occurs, but the other half will get some combination of flashes in the peripheral vision, new floaters, and possibly a curtain creeping across the vision – which is a retinal detachment until proven otherwise.
The retina is like photographic film in a camera in the back of the eye that lets you see. About 15% of patients with flashes and floaters will have retinal breaks, and about half of patients with untreated retinal breaks will develop a retinal detachment. This is important because retinal detachment is a typically a blinding condition if left untreated.
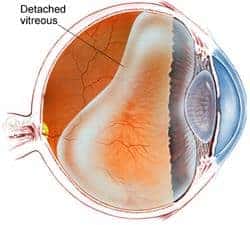
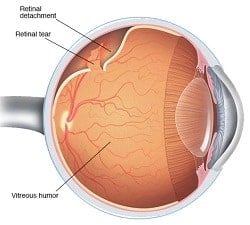
Floaters are often described as mobile shapes in the vision like cobwebs or insects and are generally due to ageing of the vitreous gel within the eye. Vitreous makes up 80% of the eye’s volume and undergoes changes throughout life. It is about 99% water and 1% fibres with a few cells. With age, the vitreous gel begins to liquify, forming pockets of fluid and clumps of fibres. Ultimately the vitreous collapses in on itself and peels away from the retina (‘PVD’, Figure 1). Most of the time no issues arise with PVDs, however uncommonly retinal tears may develop in areas where the vitreous is very adherent to the retina. This allows fluid to enter the space between the retina and its supporting wall, forming a retinal detachment (Figure 2).
Most people have some floaters, but new floaters may indicate something new has happened like a bleed in the eye or a tear in the retina. Other causes of floaters include inflammation, infection, and calcification.
Flashes
Flashes are described as peripheral arcs of light most noticeable at night. The retina is a thin tissue that lines the back of the eye and is responsible for collecting and converting light to electrical signals and then forming an image to be sent to the brain for further processing. It is similar to the film in a camera or a sensor in digital cameras. Flashes can occur with PVDs, retinal tears or retinal detachments, therefore a careful and thorough examination is required to identify the cause.
Risk Factors for Retinal Detachment
- Increasing age
- Near-sightedness (myopia) – the greater the degree, the greater the risk
- Blunt trauma to the eye
- Retinal tears or detachment in the other eye
- Previous ocular surgery
- Family history of retinal detachments
Treatment
- PVD – most commonly no treatment is necessary following a thorough retinal examination. Flashes usually resolve over days or weeks but can persist for many months in some patients. Whilst most patients become less aware of the floaters over time, some may remain. In rare instances, the floaters can be debilitating and surgical removal can be arranged with excellent results (but with some risks) – an operation called vitrectomy.
- Retinal tears – if a tear is found, then laser surgery is recommended to reduce the risk of retinal detachment. Laser treatment seals around the tear like ‘spot welding’, preventing any fluid entering the space behind the retina. Laser treatment reduces the risk of retinal detachment from about 50% to about 5%, so some patients will still require further surgery.
- Retinal detachment – if present, surgery is required to restore vision and prevent permanent loss of vision. [See section on retinal detachment for more information]
Key Points
- Flashes and floaters are usually benign but can be associated with retinal tears or retinal detachment which requires intervention to prevent loss of vision
- Careful examination by your ophthalmologist is the only way to confidently identify these issues
Contact us to get help with any questions you may have, or support you may need.

