Cataract Definition
A cataract is what we call the lens in the eye when it goes cloudy. The lens is about the size and shape of a Smartie and sits behind the iris, the coloured part of the eye. The lens helps focus light on the retina, which is the film in the camera in the back of the eye that lets you see. In younger patients, the lens changes shape to allow you to read, but this ability is lost by around 50 years of age.
Causes
Cataract development is a normal ageing process that typically takes many years but can occur faster following injury or previous eye surgery (particularly vitrectomy), and in diabetics and those taking steroid medication. In rare instances, babies can be born with cataracts.
Treatment
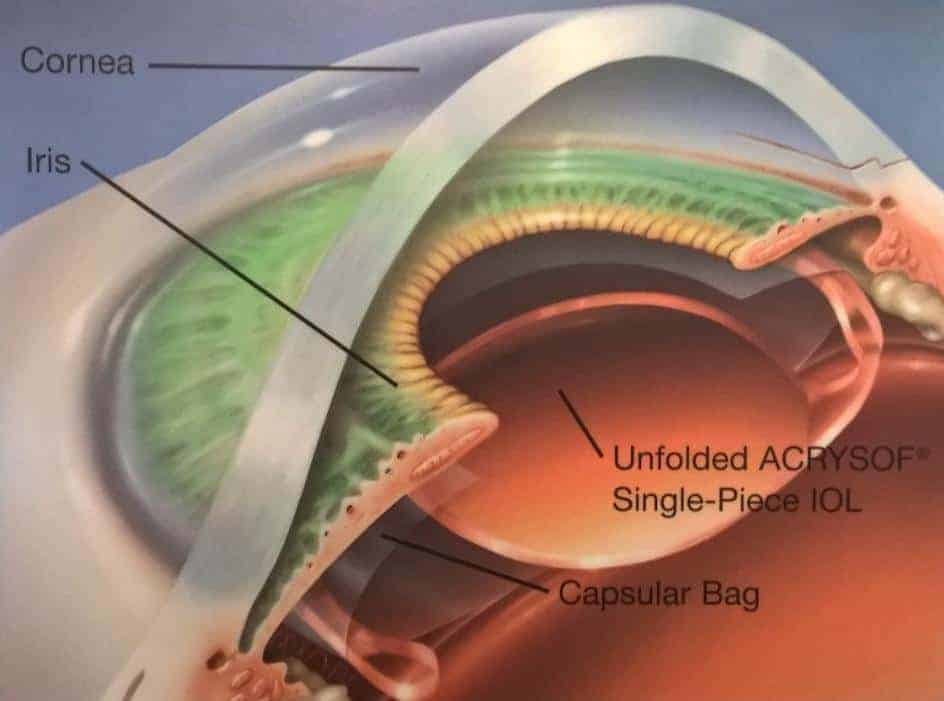
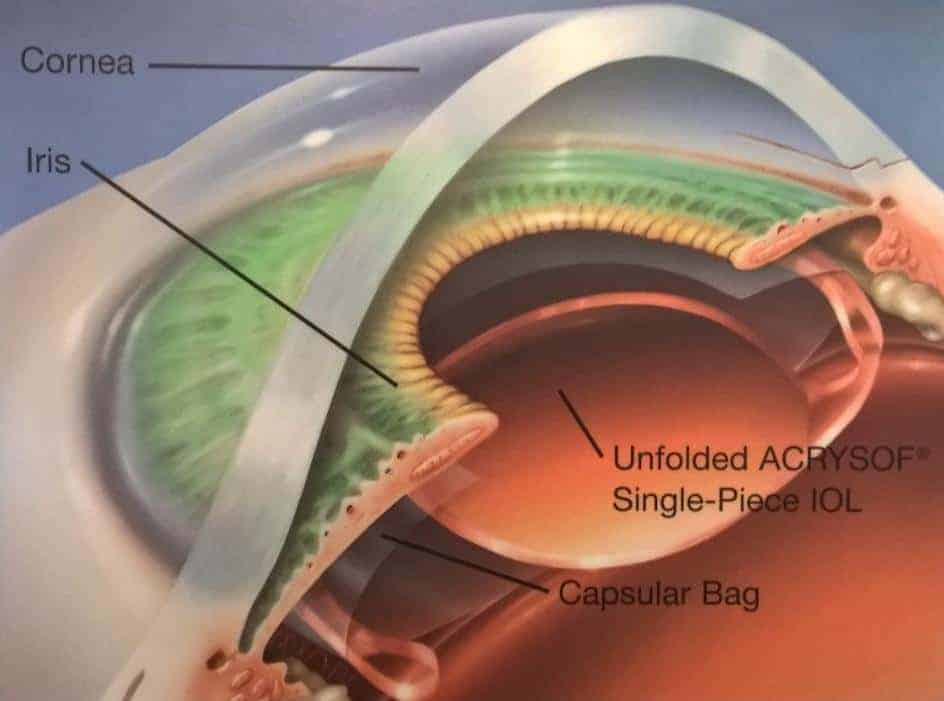
Cataract surgery involves removing the cloudy lens through tiny incisions in the wall of the eye and replacing it with a clear plastic (‘acrylic’) intraocular lens, known as an ‘IOL’. The procedure is performed in an operating theatre under sterile conditions using a special microscope. As such, cataract surgery is a form of microsurgery. An ultrasound instrument vibrates very quickly, breaking up the cataract into tiny pieces which are then removed. The new intraocular lens is carefully injected into the eye and it opens up like a ship in a bottle. The incisions are usually so small that they rarely need any stitches to keep them closed at the end of the procedure.
Timing of Surgery
The need for surgery depends predominantly on the patient’s symptoms and level of vision, but other factors such as drivers licence and occupational requirements as well as other ocular and general health issues may factor in decision making.
Benefits of Surgery
Left alone, cataracts typically cause gradual loss of vision along with a shift in the glasses prescription. Cataract surgery is highly successful in removing the cataract and improving the vision, and has the added benefit of customising the glasses prescription through the choice of IOL.
Intraocular Lens (IOL) Options
Your surgeon will talk you through the various IOL options and make recommendations based on your particular case. Broadly speaking, they can be broken down into the following:
Monofocal IOLs – both eyes are set for distance vision. This gives the clearest vision but has the relative inconvenience of needing glasses, at least for reading. (Rarely, patients may opt to have both eyes set for near vision and wear glasses for distance).
Monovision – one eye is set for distance vision and the other is set for near, aiming to reduce the need for glasses. It is best reserved for patients who have experienced it before (e.g. in contact lenses), and downsides include reduced depth perception.
Multifocal IOLs – increasingly common, multifocal IOLs give patients distance and near vision with both eyes at the same time, aiming to reduce the need for glasses. The brain makes sense of this ‘simultaneous vision’ concept in the vast majority of patients. Haloes around lights at night are common, although most patients become less aware of this over time.
Please note: with all of these options, this represents a ‘target’ we try our best to achieve within the limits of current technology, but some patients will require glasses or other procedures to fine-tune their vision postoperatively. How close to the mark we achieve mostly depends on how your eye heals up after surgery, which varies a little from one patient to the next. We cannot guarantee a particular glasses prescription outcome.
Contact us to get help with any questions you may have, or support you may need.

